MYOMECTOMY
Myoma Removal or Myomectomy
Myomectomy is a surgical procedure to remove uterine fibroids, also called fibroids. These tumors are benign, very common, and occur in the uterus. Uterine fibroids usually develop during the childbearing years, but can occur at any age.
The surgeon’s goal during myomectomy is to remove fibroids that are causing symptoms and reconstruct the uterus. Unlike a hysterectomy, in which the entire uterus is removed, a myomectomy removes only the fibroids and leaves the uterus.
Women who undergo myomectomy have a great improvement in their symptoms, including a decrease in heavy menstrual bleeding and pelvic pain.
Why is it done?
Myomectomy is recommended when they cause symptoms that are troublesome or interfere with normal activities. If you need surgery, reasons for choosing myomectomy over hysterectomy for uterine fibroids include the following:
Planning to have children. Your doctor thinks that fibroids or uterine fibroids may be interfering with fertility. You do not want to lose your uterus.
Risks: Myomectomy has a low complication rate. Still, the procedure presents a number of unique challenges. Risks of myomectomy include: Excessive blood loss. Many women with uterine fibroids already have a low red blood cell count (anemia) caused by heavy menstrual bleeding, so they are more at risk for problems due to blood loss.
During myomectomy, surgeons take extra steps to prevent excessive bleeding. Some of these include blocking the flow of uterine arteries with tourniquets and clamps and injecting medicine around the fibroids so that the blood vessels don’t bleed as much.
Scar tissue. Incisions inside the uterus to remove fibroids can lead to adhesions-bands of scar tissue that may develop after surgery. Laparoscopic myomectomy may cause fewer adhesions than abdominal myomectomy (laparotomy). To choose between these two techniques, the gynecologist will perform a preoperative evaluation to determine which technique is more convenient.
Complications in pregnancy or childbirth. A myomectomy may increase certain risks during childbirth. If the surgeon had to make a deep incision in the uterine wall, the doctor monitoring the pregnancy might recommend a cesarean delivery to avoid tearing of the uterus during labor, a very rare complication of pregnancy. Fibroids or fibroids themselves are also sometimes associated with pregnancy complications.
Very remote possibility of a hysterectomy. The surgeon should rarely remove the uterus if the bleeding is uncontrollable or if abnormalities other than fibroids are found. This is very rare with a surgeon who has extensive experience in the technique and has a rigorous protocol that involves maximizing success.
What recommendations should I follow after the procedure?
Upon discharge from the hospital, your doctor prescribes oral pain medication, prescribes care, and discusses diet and activity restrictions. You can expect vaginal spotting to occur for a few days and for up to six weeks, depending on the type of procedure you had.
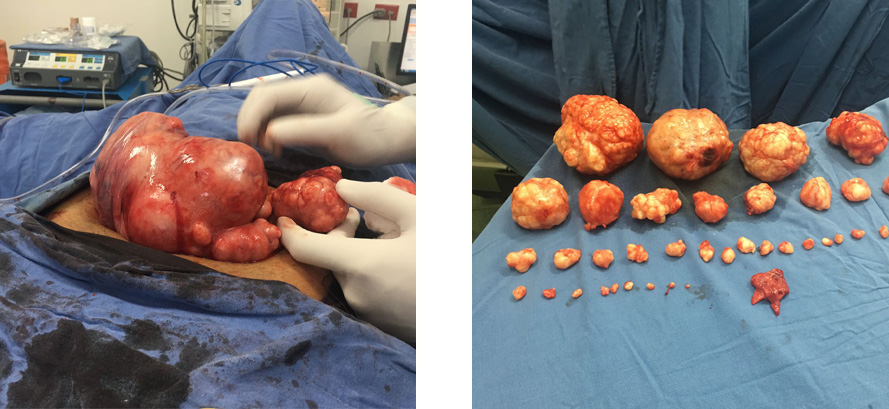
What results can you get with myomectomy?
Symptom relief. After a myomectomy, most women experience relief from bothersome signs and symptoms, such as excessive menstrual bleeding, pelvic pain and pressure.
Improved fertility. Women who have a myomectomy have good pregnancy outcomes within approximately one year after surgery. After a myomectomy, a waiting time of three to six months is suggested before attempting conception to allow the uterus to recover.
Fibroids that are missed by your doctor during surgery, or that are not completely removed, may eventually grow and cause symptoms. New fibroids may also develop, which may or may not require treatment. Women who have had only one fibroid have a lower risk of developing new fibroids, often called a recurrence rate, than women who have had multiple fibroids. Women who become pregnant after surgery also have a lower risk of developing new fibroids than women who do not become pregnant.
What kind of preparation should I consider?
You will need to fast, not eat or drink anything, for a few hours before surgery. Follow your doctor’s recommendation for the specific number of hours.
If you are taking medications, check with your doctor to see if your usual medication routine should be changed in the days leading up to surgery. Tell your doctor if you are taking any over-the-counter medications, vitamins, or other dietary supplements.